Myxofibrosarcoma Tumor Removal Patient Testimonial
- What is Myxofibrosarcoma cancer?
- What Are Treatment Options for Myxofibrosarcoma?
- What is Recovery Like After Tumor Removal Surgery?
When Marla noticed a small lump on her leg at the gym, she never would have imagined it to be one of the most aggressive forms of soft-tissue tumors.
Shortly after her primary care physician ordered an MRI, Marla was diagnosed with myxofibrosarcoma, a rare form of cancer that develops in fibrous (connective) tissue, usually just under the skin of the arms and legs.
Fearing the worst, and in a determined effort to save her life, Marla turned to Craig P. Jones, M.D., a board-certified orthopaedic surgeon specializing in orthopaedic oncology at the Orlando Orthopaedic Center, to surgically remove the fast-growing tumor.
“The biggest benefits of the surgery were that I got to keep my leg, no amputation,” says Marla. “Dr. Jones saved my life.”
What Is a Myxofibrosarcoma?
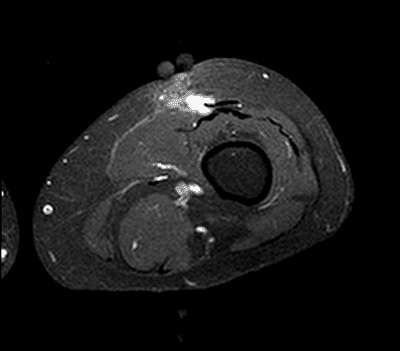
MRI scan of Marla’s tumor.
Myxofibrosarcoma (MFS) is a variation of the group of malignant fibrous histiocytomas, a type of cancer that forms in the soft tissue and the bone. MFS can occur anywhere in the body but often manifests in the legs. MFS is one of the rarer soft-tissue sarcomas. However, its aggressive nature makes it particularly dangerous because it can be tricky to diagnose and detect properly.
Marla’s experience was a case in point. When she first noticed the bump on her leg, its normal-looking appearance did not give her cause for alarm. “In May 2015, I was getting off my treadmill and noticed a small lump on my leg when I was wiping down,” says Marla.
“I didn’t think anything of it, but the next week I noticed that the lump had gotten larger. I went to my primary care physician, and she asked me to get an MRI. When the MRI came back, she noticed that the outer perimeters of the tumor looked suspicious in their size and growth. I was diagnosed with a myxofibrosarcoma above my left knee.”
The visible part of the initial MFS growth can often represent only a portion of the underlying tumor, which may have expanded significantly down into deeper tissue. Even with the most advanced imaging techniques, it can be challenging to identify the complete scope of cancer.
A physician may be alerted to the presence of MFS when the tumor is:
- As large as a golf ball
- Gets bigger over time
- Lies deeper in the muscles instead of superficially
What Are Treatment Options for Myxofibrosarcoma?
 Several factors influence the precise treatment needed for MFS including:
Several factors influence the precise treatment needed for MFS including:
- The depth of the tumor
- Size – larger tumors may need more extensive surgery, radiation treatment or chemotherapy.
- Grade – MFS can contain different levels of aggressive dividing cells. A low-grade tumor with more inactive cells will receive different treatment than a high-grade tumor containing higher amounts of dividing cells.
- Previous treatment – MFS can recur as a result of prior radiation treatment. When it does, the second tumor often has a higher grade than the first.
Surgery is always required to remove the tumor and some normal tissue that surrounds it. Radiation therapy is typically administered after surgery. Some smaller, low-grade, and surface MFS tumors may only need surgery if the cancer is not located close to a joint or other critical bodily structures.
Traditionally, almost half of MFS patients underwent amputation of the diseased limb to completely remove the tumor and prevent a recurrence of cancer. However, with the advances in modern surgical techniques, orthopaedic oncologists make it a priority to preserve a patient’s limb whenever possible.
Given the aggressive nature of Marla’s tumor, Dr. Jones decided to perform chemotherapy before surgery and radiation treatment following the procedure.
“I first saw Marla about a month after she developed a mass above her knee, just above her knee in the medial left thigh,” says Dr. Jones. “She had an MRI which showed a mass inside of the quadriceps muscle.”
“Marla underwent two cycles of chemotherapy. A repeat MRI showed that the mass had gotten smaller which made the surgery less invasive. After surgery, Marla underwent radiation therapy to reduce the likelihood of local recurrence.”
Marla was impressed by Dr. Jones’ professionalism, his understanding of the body, and his candid, genuine bedside manner. “He’s very professional and very knowledgeable,” says Marla. “Dr. Jones understands the workings and the biology of the body. He’s no-nonsense and will tell you right up front what needs to be done, what can be done, and give you your options.”
What is Recovery Like After Tumor Removal Surgery?
 An integral part of the healing process after surgery it to follow a rehabilitation program under the guidance of an experienced and skilled physical therapist.
An integral part of the healing process after surgery it to follow a rehabilitation program under the guidance of an experienced and skilled physical therapist.
“After surgery, Marla underwent physical therapy to get her motion back,” says Dr. Jones. “And months after completion of radiation therapy has now returned to full activity, including running.”
“After my surgery, I did physical therapy,” says Marla. “I trained to walk again, and I recently did my first marathon, and completed the Disney marathon. Now I’m training to run again; I just completed my first 10k running in about an hour and 9 minutes.”
After her successful tumor removal surgery, Marla is thankful for all the people who helped her along her healing journey and plans to experience and savor every active moment that life has to offer.
“I credit a lot of people for saving my life,” says Marla. “Number one, my primary care physician who told me to get checked in the first place, myself for noticing (laughs), and Dr. Jones. From here on out, I go different places and try different things. I did a 30-day yoga challenge to see if I could accomplish that. I did CrossFit for six weeks, and I’m doing the Orangetheory workout now. So I see what I can do to push my limits.”


