How Can a Robot Help Surgeons Deliver Better Hip and Knee Replacements?
Dr. Bonenberger and Dr. Van-Dyke Mako robotic arm
Having a robot and 3D computer software help your surgeon design and place a perfect-fitting implant to replace your knee and hip joint may have seemed like something out of a science fiction movie just a few years ago, but today it is science fact.
MAKO robotic-arm assisted surgery helps surgeons ensure patients will receive a custom-fit partial knee or hip replacement resulting in faster recovery, less pain and less stress. In fact, many patients are able to return home the same day as the surgery thanks to the technology.
Eric G. Bonenberger, M.D., a board-certified orthopaedic surgeon specializing in minimally invasive joint replacement surgery, was instrumental in bringing the technology to the Orlando Health Dr. P. Phillips Hospital (DPH). He, along with Travis B. Van Dyke, M.D., chief of surgery at DPH, were featured in the most recent issue of the Southwest Orlando Bulletin to discuss the technology and what it means for patients.
Fellowship trained at Boston University, Dr. Bonenberger is one of the few surgeons in the state of Florida certified in all three Mako platforms (partial knee, total knee, and total hip arthroplasty), and he has been utilizing computer-assisted surgery and MAKO robotic technology since 2006.
“Compared to traditional instrumentation, what the surgeon and patient realize in using this technology is it improves your understanding of all the different parameters you have to account for when you are performing the surgery,” says Dr. Van Dyke. “It makes the surgery easier, quicker, and more precise than traditional instrumentation.”
How Does MAKOplasty Technology Work?
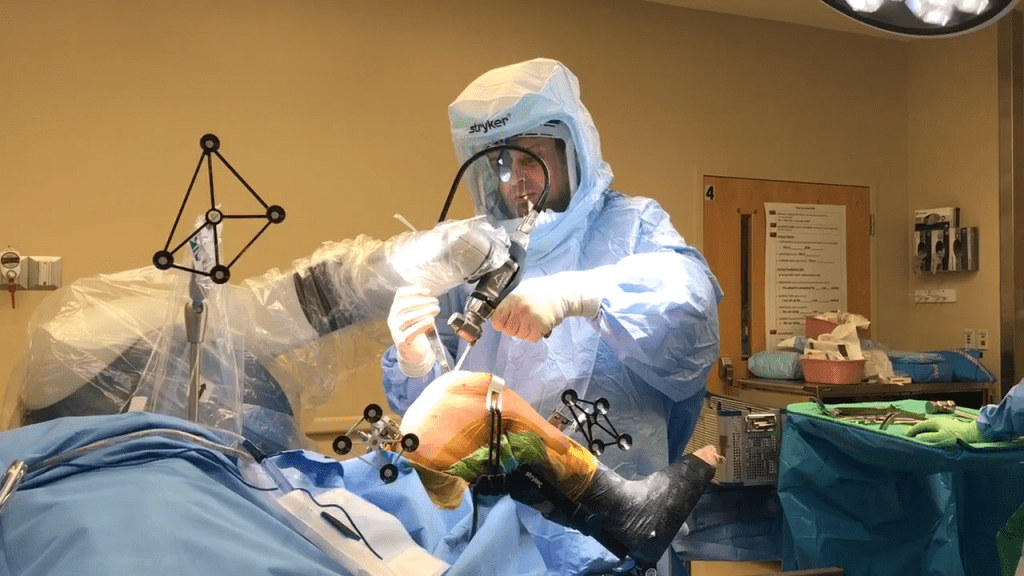
Dr. Bonenberger Mako robotic arm
The MAKO robotic-arm from Stryker has revolutionized the success rates of partial knee, total knee and total hip replacement surgeries. It helps orthopaedic surgeons who have been specially trained to use the robot perform minimally invasive partial joint replacements in targeted areas with smaller incisions and more accuracy than traditional surgery.
Surgeons must screen potential candidates to ensure they are eligible for MAKO surgery through a series of tests and an evaluation of each patient’s medical history. After that, preparation for a MAKOplasty partial or total knee or hip replacement starts well before the patient steps foot in the operating room.
MAKO technology provides the surgeon with a patient-specific 3D model to pre-plan their joint surgery. The surgeon is also able to visualize and adjust the joint before surgery by moving the patient’s knee or hip through various range of motion exercises. The final plan is then programmed into the robot’s computer navigation system in preparation for surgery.
During the procedure, the surgeon uses the MAKO robotic-arm to replace the specific area of the knee or hip causing the pain. Throughout the procedure, the doctor is in complete control of the robotic arm and the arm’s navigation system provides real-time sensory feedback, to ensure proper preparation of the bone, and correct, pinpoint placement of the implant.
“MAKO technology allows us to map out the area where the surgery will be performed and make adjustments as needed in the operating room,” says Dr. Bonenberger. “The surgeon is in complete control and we move the robot arm to assist with joint placement, helping provide the very best results for patients.”
What Are the Benefits of MAKO Robotic Arm Technology?
Thanks to a more accurate placement of the implant, patients experience shorter hospital and recovery times, and some patients can even avoid an overnight hospital stay altogether.
“The MAKO robotic-arm provides surgeons with a degree of security and comfort unavailable in the past regarding the planning and the implementation of surgery,” says Dr. Bonenberger. “With the increased precision, hip and knee implants can potentially last 20 to 30 years instead of 10 to 20.”
Through the combined forces of surgeon and robot, adult patients who meet the right criteria are able to leave the hospital sooner, with less stress, decreased post-surgical pain and a faster way to begin enjoying life again.
The robotic arm (seen above covered in plastic) is used to assist Dr. Bonenberger complete the surgery. Real-time video feedback is seen on a screen across from Dr. Bonenberger.
The first ever Mako Robotic Total Knee Replacement preformed at Dr. P. Phillips Hospital was recently completed by Dr. Bonenberger.


