How Is the iFuse Implant System Revolutionizing Sacroiliac Joint Fusion Surgery?
- Why Would a Patient Need SI Joint Fusion Surgery?
- What Are New Vs. Old Methods of SI Joint Fusion Surgery?
- How Do You Prepare for iFuse Implant System Surgery?
- How Is iFuse Implant System Surgery Performed?
- What Are the Results of the iFuse Implant System?
The iFuse Implant System is a minimally invasive approach for sacroiliac (SI) joint fusion surgery to relieve sacroiliac joint pain and treat conditions, including sacroiliac joint disruptions and degenerative sacroiliitis. The procedure utilizes a smaller incision and a guide pin to provide stability to the SI joint, which results in less pain and quicker recovery time for patients.
Available since 2009, the iFuse Implant System is designed to provide immediate SI joint stabilization and allow long-term fusion.
Why Would a Patient Need SI Joint Fusion Surgery?
“A patient would be recommended for SI surgery when they exhibit symptoms of chronic sacroiliac inflammation and degeneration, and when conservative methods of treatment – such as medication, therapy and injections – have failed,” says G. Grady McBride, M.D., a board-certified orthopaedic surgeon specializing in cervical and lumbar spinal surgery at Orlando Orthopaedic Center.
“SI joint dysfunction, when the sacral bone joins the pelvis bone, may lead to pain in the lower back or upper buttock area. The pain is fairly common, and frequency does increase with age.”
What Are New Vs. Old Methods of SI Joint Fusion Surgery?
The traditional SI joint fusion surgery involved open surgery that could last up to several hours, required a large incision and a prolonged hospital stay and recovery. The surgeon would remove cartilage tissue from the joint and use bone grafts from another part of the body to help fuse the SI joint.
With the iFuse Implant System, patients no longer have to endure much of the discomfort and inconvenience experienced with the traditional procedure. iFuse SI joint fusion surgery requires a very small incision. It uses a special guide pin to place rigid titanium implants specifically made to stabilize and fuse the heavily loaded SI joint. These small implants are designed to stabilize the SI joint and allow healing through the minimization of micromotion.
“The advantages to the patients are that, as a minimally invasive procedure, the recovery is quite rapid, and you’re out of the hospital the next day with minimal downtime,” says Dr. McBride. “Patients can be up walking the evening of surgery with a walker, and they will only need to limit weight-bearing for approximately three weeks.”
SI joint dysfunction is quite common in patients who have undergone lumbar fusions. In fact, some studies have indicated up to 50 percent of patients having lumbar fusions or lumbosacral fusions develop degeneration in the adjacent sacroiliac joints. With the iFuse system. there are no conflicts with lumbar fusion devices, meaning if a patient previously had spinal surgery, they may still be a candidate for the new procedure.
“From a surgeon’s standpoint, the iFuse System is relatively simple and offers special targeting guides to insert the stabilizing pins which are directed under x-ray or fluoroscopic control,” says Dr. McBride. “This limits the size of the incision needed to insert these pins, which really is a benefit for both the patient and surgeon.”
How Do You Prepare for iFuse Implant System Surgery?
The road to an iFuse Implant System starts at the initial exam. If a patient is experiencing lower back symptoms predominately below the L5 vertebra and the physician is able to determine pain originates in the SI joint, the doctor will request X-rays or a CT scan to look for signs of degeneration of the joint.
“A common test to determine whether a patient may be a candidate for SI surgery is to do a selective injection of Lidocaine or an anesthetic agent in the sacroiliac joint,” says Dr. McBride. “If the sacroiliac pain is completely relieved for several hours, then that would indicate the source of the pain and suggest they may benefit from the iFuse Implant System.”
Before surgery is considered, all conservative measures of treatment (such as the injections mentioned above and physical therapy) are attempted. Only after these measures have failed will a patient be considered for surgery.
How Is iFuse Implant System Surgery Performed?
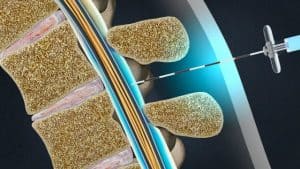
Injection prior to iFuse Implant System surgery
If the patient chooses to undergo the iFuse surgery to stabilize their SI joint, the patient will be contacted by the physician’s office, and surgery will be scheduled. On the day of the operation, the patient will be admitted and administered a general anesthetic.
They will then be placed lying face down on the surgical table while the surgeon uses the specially designed iFuse system to guide the instruments that prepare the bone and insert the implants. The entire procedure is performed through a small incision (approximately 2-3cm long) along the side of the buttock. During the procedure, X-ray guidance provides the surgeon with live imaging to facilitate the proper placement of the implants. Typically three implants are placed, depending on the patient’s size. Surgery is usually completed in less than forty minutes, and the patient is returned to their room and instructed to start limited weight-bearing activities shortly after surgery.
“Following surgery with the iFuse Implant System, the patient only needs to limit weight-bearing for approximately three weeks, and recovery is quite rapid with full healing in the six to eight-week timeframe,” says Dr. McBride.
Patients will return to their physician’s office between one and two weeks following surgery for a follow-up appointment to assess the incision and for follow-up X-rays. Based upon the physician’s recommendation, patients will also have to come back to the office twelve weeks post-surgery for more X-rays and to determine whether they may resume full weight-bearing activities.
What Are the Results of the iFuse Implant System?
“Overall, this system has had a very high success rate with very few failures,” says Dr. McBride. “Healing is usually complete by the six to eight-week timeframe, but I usually will limit my patients from doing anything strenuous for a three to four-month period. Hopefully, by that time, the patient has made a full recovery, and their sacroiliac pain has resolved.”



