Distal Radius Fracture
- What is a distal radius fracture?
- What are the symptoms of a distal radius fracture?
- What is the treatment for a distal radius fracture?
Fractures of the distal radius, or wrist fractures, account for about 20% of all emergency department visits in the United States every year. These types of fractures make up about 8-15% of all bone-related injuries annually in the U.S.
Many times, these fractures are associated with falling, with your hand and wrist taking the full force of pressure from the fall. How are these fractures treated and what are your chances of recovering fully from the injury?
What is a Distal Radius Fracture?
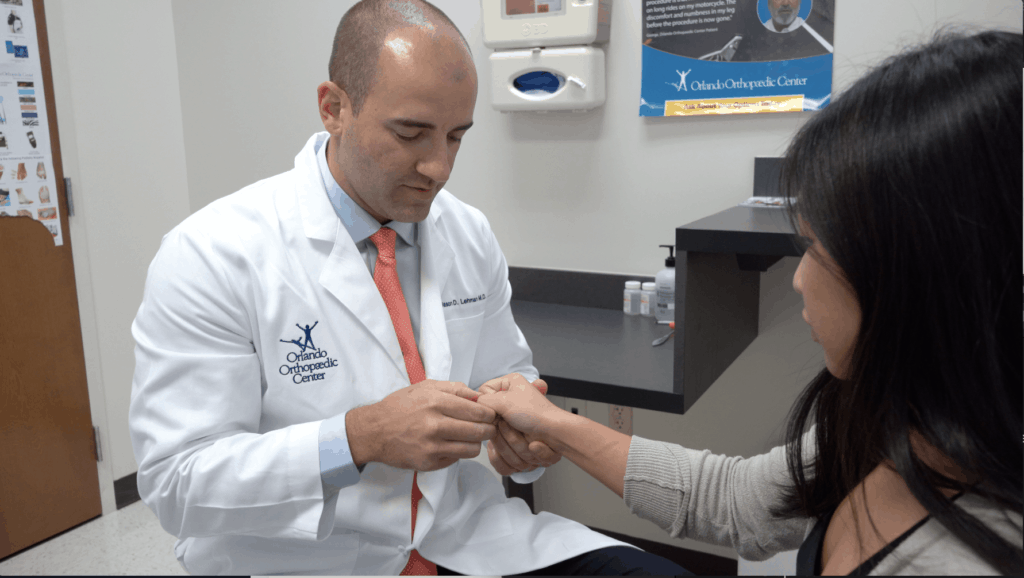
A distal radius fracture involves injury to one of the bones of the wrist. Jason D. Lehman, M.D., a hand and upper extremity orthopaedic surgeon at the Orlando Orthopaedic Center, commonly treats the condition known as a distal radius fracture. He explains that, “The forearm is actually comprised of two bones, both the radius and ulna. The radius is commonly fractured at its distal end, right at the wrist. This is one of the most common fractures that we see in all of orthopaedics.”
Distal radius fractures usually occur with a fall onto an outstretched hand. This can occur during bike accidents, sporting activities, or simple falls. These fractures can happen to anyone. Dr. Lehman states that a distal radius fracture, “Happens in both very young patients as well as older patients. It’s slightly more common in women and can sometimes be a sign of osteoporosis or low bone density.”
What Are the Symptoms of a Distal Radius Fracture?
If you’ve suffered a distal radius fracture, the chances are high that you’ll know it immediately. Patients often experience these symptoms:
- Significant wrist bruising and swelling
- Pain that is worsened by grip
Obvious deformity at the wrist
When a wrist injury occurs it can be difficult to know if you have a sprain or an actual fracture. A sprain affects the underlying ligaments, where a fracture actually breaks the bone. Both can be very painful conditions that require treatment from a specialist in this area.
However, if your wrist appears deformed and you have pain, bruising, and swelling, the chances are high that you’ve suffered a distal radius fracture.
Dr. Lehman says, “Patients with this disorder often present with pain and sometimes deformity at the wrist. It’s very important to have a consultation with a hand and wrist surgeon to discover different treatment options.” It’s important not to wait; you don’t want the bone to begin to heal in the wrong position.
What is the Treatment for a Distal Radius Fracture?
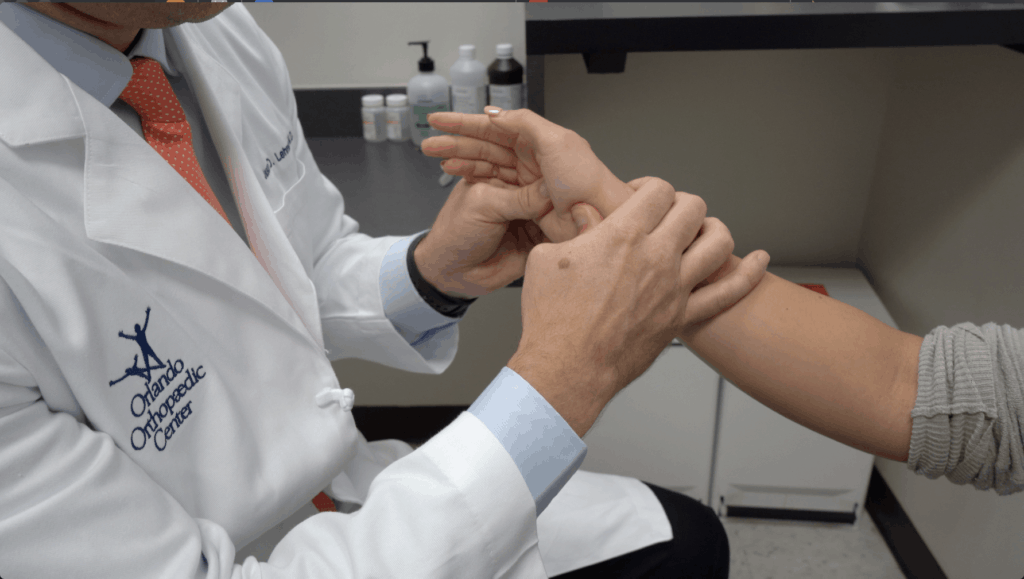
Consulting with a hand and upper extremity specialist like Dr. Lehman is the first step toward recovery. Your individualized treatment plan depends on a number of factors, including:
- If the bone is displaced and if so, to what degree
- Whether the joint was involved
- Whether nerves were affected
- If this is your dominant hand
- Your occupation, age, and activity level
Dr. Lehman notes that, “Sometimes based on the fracture pattern, as well as the patient’s desires, these are treated nonoperatively with a period of immobilization with a cast or split. Other times they require surgery in which we open up the fracture, reduce it into its anatomic position, and then fix it with a combination of plates and screws.”
If you and your doctor elects for nonsurgical treatment of the distal radius fracture, it may require the fracture to be realigned before putting it in a cast or splint. This occurs under local anesthesia to numb the painful area. Then the cast or splint is placed and typically left on for up to six weeks to allow the injury to heal. X-rays will be taken at diagnosis and potentially throughout the healing to monitor your progress. You may then wear a removable wrist splint and undergo physical therapy to regain wrist strength and full function.
If your distal radius fracture can’t be treated with just a cast, your orthopaedic surgeon will schedule surgery to repair the injury. These surgeries are usually performed under regional anesthesia. The surgeon will male an incision at the wrist, and reduce the bones to their anatomic position. As Dr. Lehman indicated, a combination of pins, screws, and plates are then used to hold the bones together.
After surgery, a splint is placed on the wrist. You will see the doctor at 1-2 weeks postoperatively for a wound check. You will then begin work with a certified hand therapist to work on range of motion and strengthening of the wrist. Your hand therapist will also provide you with home exercises to help regain all the function you had before the injury.
Dr. Lehman reports, “You will be able to use your hand and fingers for normal activities immediately after surgery, but typically, patients require about three months after surgery before they have full use of the upper extremity.”


