Can Bunionectomy Surgery Help Patients Walk Pain-Free Without Compromise?
- What Are Bunions?
- What Are the Treatment Options for Bunions?
- How Is a Bunionectomy Performed?
- What Is the Recovery Like After Bunionectomy?
A bunionectomy surgery may help patients walk pain-free without compromise depending on a variety of factors.
For Kathy, the pain around her big toe joint got so bad she couldn’t wear sneakers or athletic shoes without experiencing extreme discomfort.
After consulting with two other orthopaedic practices, Kathy turned to Daniel L. Wiernik, D.P.M., a board certified surgeon specializing in foot and ankle surgery, podiatry, and reconstructive rearfoot/ankle surgery at Orlando Orthopaedic Center.
“The biggest benefit for me was taking my life back and being pain-free,” says Kathy. “It was really bad. The pain was raw before surgery. I don’t have that pain anymore.”
What Are Bunions?
Individuals, mainly women, who grow up wearing restricted and cramped footwear can develop swelling that affects the base of the big toe. Over time, a bony, lumpy protrusion known as a bunion can develop, causing enlargement of the big toe joint. This, in turn, causes the big toe to curve out towards the other toes of the foot and make the skin covering the bunion become red and sore.
The Podiatry Institute reports that bunions are one of the most common structural deformities seen in podiatric medicine, with over 150,000 bunion surgeries performed every year in the U.S. Bunions are often passed down from parents to children especially among individuals with low arches, flat feet, and loose joints and tendons. More than 35% of people over the age of 65 have at least one bunion.
The more exacerbated the angle and size of the bunion the more pain can be experienced by patients when walking or putting weight on their feet, particularly in tight shoes such as high-heels. As a bunion alters the foot’s bone structure, it can severely hinder one’s ability to walk and also cause additional damage to other toes such as calluses, hammertoes, and ingrown nails. Bursitis or arthritis can also result from the damage if left untreated.
What Are the Treatment Options for Bunions?
Daniel L. Wiernik, D.P.M., bunionectomy
Patients experiencing the early stages of bunions have a variety of conservative treatments available to them:
- Shoes with wide toe boxes and without elevated heels that allow the foot to spread
- Massage therapy and range of motion exercises
- Wearing orthotic shoe inserts to recoup proper foot balance
- Sleeping with a splint to help straighten out the toe joint
- Icing the bunion or soaking the foot in warm water
Patients who suffer stubborn and relentless pain due to a swollen big toe joint may need to opt for surgery (known as a bunionectomy) to have the bunion removed.
For Kathy, when the pain became unbearable even when she was wearing her most comfortable shoes, she chose to have a bilateral bunionectomy to remove the bunions.
“It got so bad that at one point I was in pain even in sneakers and walking shoes. I learned from Dr. Wiernik that my women’s footwear was contributing to my issue, wearing heels and things with high arches. When it got to the point where I couldn’t walk without being in pain in athletic shoes, I knew I had to do something.”
In fact, Kathy required a bilateral bunionectomy, where bunions on both feet are removed during two different procedures.
How Is a Bunionectomy Performed?
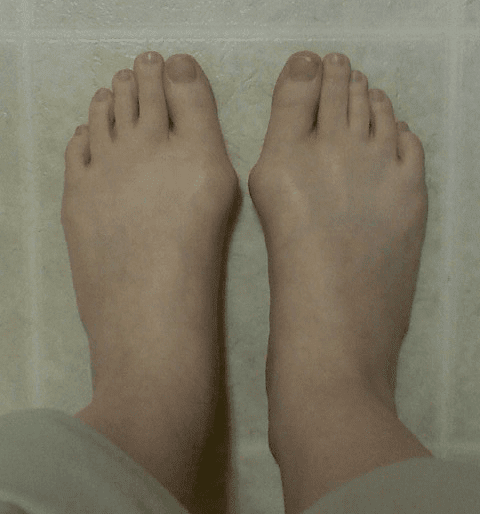
Kathy Pre-bunionectomy Surgery
A bunionectomy is performed as outpatient surgery, and patients, for the most part, can return home the same day. Bunions have unique characteristics and come in different shapes and sizes. As such, a variety of surgical procedures can be performed to alleviate them. In general, a surgeon will correct the alignment of the big toe bone and repair the soft tissue surrounding it.
The primary surgeries for repairing bunions include:
Osteotomy
The surgeon realigns the big toe joint by making tiny cuts in the bones and then stabilizing the new alignment with state-of-the-art pins, screws, or plates. As part of the procedure, the doctor may remove a bump from the joint (known as an exostectomy).
Arthrodesis
Used primarily for patients with serious arthritis or severe bunions, the surgeon will remove the arthritic joint surface and insert screws, wires, or plates to keep the bones in place until they fuse together.
The decision to undergo surgery is a major one. An essential part of the decision-making process is choosing a proficient surgeon that inspires comfort and confidence in the patient.
Kathy felt an instant connection and rapport with Dr. Wiernik that she didn’t have during her two prior visits to other practices. “Immediately sitting down with Dr. Wiernik, it was such a better experience than the practice I went to for a first opinion and with another practice that I tried to get a second opinion with,” says Kathy.
“He was really great about not disparaging the first doctor’s opinion but telling me the medicine behind why he completely disagreed.”
What Is Recovery Like After Bunionectomy?
Kathy after Bunionectomy surgery
As with any surgery, each patient’s recovery depends on the individual’s overall health and medical history, the degree of bunion deformity, the patient’s age and lifestyle. Most patients will typically require a fracture shoe for up to a month after surgery. Occasional swelling in the foot may be felt for several months afterward.
After the incision heals, your surgeon may recommend a range of motion and strengthening exercises to bolster foot stamina and resilience. Patients are normally back to their daily routine activities within two months after surgery.
Kathy was a fitness instructor and maintaining her active lifestyle was very important to her. “I had been teaching fitness classes which I didn’t want to give up, but I knew I needed surgery on both feet,” says Kathy. “I did it one foot at a time, and I was back teaching my classes within twelve months.”
“I was thrilled to have less than a year of downtime. When teaching indoor cycling classes, all the pressure is on the balls of your feet when you’re in those pedals,” Kathy continues. “Here I am still teaching indoor cycling classes.”
The American Orthopaedic Foot and Ankle Society confirms that procedural complications were seen in less than ten percent of bunionectomy patients, and patients reported an 85–90% success rating for the procedure.
“I would say to anyone considering having this surgery, do your homework, decide if you can live with the pain or not,” says Kathy. “Know that bunions will progress, they will get worse. There is nothing you can do outside of the surgical intervention to fix it or to help remediate what’s happening in the joint. Go for multiple opinions if you need to, and feel comfortable that what you’re being told is the best thing out there for you.”
After her successful bilateral bunionectomy, Kathy wholeheartedly recommends Dr. Wiernik and his staff to anyone needing similar treatment. “I very much recommend Dr. Wiernik and his team,” says Kathy. “I felt like I was very well taken care of from beginning to end. I had both feet done with him. I was comfortable in round one, and I came in even more comfortable in round two, as I knew what I was working with. I just felt that they really accepted me as a patient and I felt very connected to Dr. Wiernik and his staff.”


