Can Epidural Steroid Injections Help Relieve Pain Without Surgery?
- What is an Epidural Steroid Injection?
- How is an Epidural Steroid Injection Performed?
- How Effective is an Epidural Steroid Injection?
When visiting with a pain management physician in Orlando, treatment may include physical therapy, therapeutic modalities, prescription medication and/or interventional pain management consisting of epidural steroid injections.
Although some consider epidural steroid injections a “last resort” of sorts in the pain management subspecialty, patients report high satisfaction and effectiveness ratings.
“I compare it to putting the water where the fire is,” says Daniel M. Frohwein, M.D., a pain management physician at Orlando Orthopaedic Center. “I would rather target the medication right at the pain generator rather than prescribe the medication orally, only to have a fraction of the medication reach the problem area.”
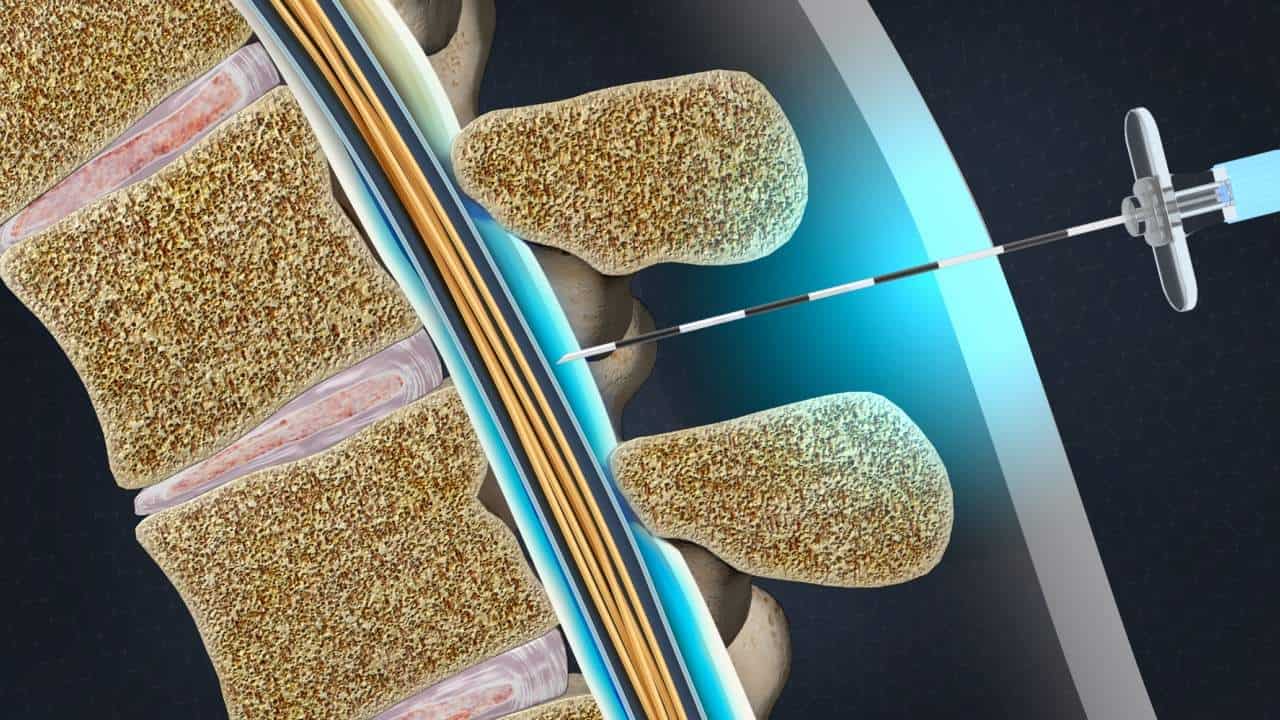
What is an Epidural Steroid Injection?
An epidural steroid injection is a minimally invasive procedure used by pain management physicians to relieve both spine and extremity pain caused by disc herniation, disc degeneration, spinal stenosis, and inflamed nerve roots.
“The medication is delivered to the inflamed spinal nerve through the epidural space,” explains Dr. Frohwein. The epidural space is the area between the protective covering of the spinal cord (the dura) and the bony elements that form the spinal canal.
The injection includes a corticosteroid (betamethasone or triamcinolone typically) and a numbing agent (bupivacaine or lidocaine).
“Corticosteroids reduce inflammation and have the potential to work very well when delivered directly to the site of pain,” says Dr.Frohwein. “Often times patients report near immediate pain relief following the procedure. If only mild relief is achieved, we may schedule one or two more injections to achieve maximum effectiveness.”
He continues, “It is important to remember, however, that an epidural steroid injection is only a method of delivering medication. It will not change lumbar spinal anatomy or increase abdominal muscle strength. Therefore, we must have close working relationships with both our spine surgery and physical therapy colleagues should additional treatment be needed.”
Dr. Frohwein that epidural steroid injections are often combined with physical therapy or home exercise programs to strengthen the back and core musculature, and to help prevent future pain.
How is an Epidural Steroid Injection Performed?
Once an epidural steroid injection has been decided as the next course of treatment for patients, they are briefed on what to expect the day of the procedure. For Dr. Frohwein, the epidural steroid injection will take place at the Orlando Orthopaedic Center Outpatient Surgery Center just south of downtown Orlando.
Using a fluoroscope (a special type of X-ray), the physician directs a hollow needle through the skin and into the epidural space. There are two techniques used to access the epidural space, either an interlaminar or a transforaminal approach.
The interlaminar approach advances a needle between the lamina of two vertebrae at the target location, through the ligamentum flavum, and into the posterior epidural space.
The transforaminal approach aims to place the needle in opening of the neural foramen. This approach allows placement of medication into the anterior epidural space and closer to the spinal nerve roots. In both scenarios, contrast dye is used to confirm proper spread of medication.
Most patients remain awake during the procedure and typically feel more pressure than pain. Some patients elect mild or even heavy conscious sedation for comfort. Once the needle is in place and the steroid medication is delivered, the needle is removed and patients are moved to a recovery area and cleared to leave shortly thereafter.
The entire procedure typically takes less than 20 minutes.
How Effective is an Epidural Steroid Injection?
Unfortunately there is not a “standard” amount of time a patient will feel relief following their epidural steroid injection. Pain relief may last for several weeks, or it may last for several years.
“Although we can’t predict how long pain relief will last, we do know that a majority of patients experience reduced pain and improved function in very short order,” says Dr. Frohwein. “At times, the response can be quite miraculous. Other times, we see only limited improvement. Much of that depends on the specific anatomy, individual physical condition, and, what I hypothesize, a large genetic component.”


