Getting Back to Work Following a Hand Tumor Removal
- What Is a Hand Tumor?
- What Are the Treatments for Hand Tumors?
- What Is the Recovery Like After Hand Surgery?
The hand tumor on Donna’s hand had grown so large it prevented her from accomplishing the most simple tasks and interfered with her ability to be productive at work.
“For about a year, I was having mobility problems working at my desk on the keyboard, and picking up a pencil,” says Donna. “(The tumor) became quite big, it was growing, and causing more problems.”
Fortunately, she found a solution when she consulted Orlando Orthopaedic Center’s Craig P. Jones, M.D., a board-certified orthopaedic surgeon specializing in orthopaedic oncology, and Alan W. Christensen, M.D., a board-certified orthopaedic surgeon specializing in hand surgery.
“Six months ago, I had surgery on my thumb, and Dr. Jones and Dr. Christensen performed it,” says Donna. “Since then, it’s been amazing. My ability to work on my keyboard has improved, my ability to write and hold a pen. I’m extremely pleased with everything that came out of having the surgery.”
What Is a Hand Tumor?
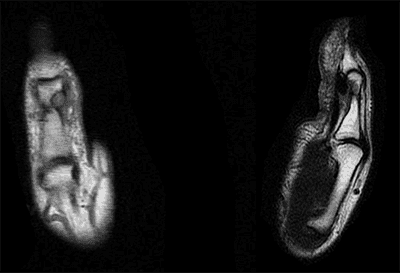
Donna MRI Scans Hand Tumor
A tumor refers to any irregular lumpy or bumpy mass in the hand or wrist. Tumors may be malignant (cancerous) or benign (non-cancerous). However, the vast majority of hand tumors (98-99%) are non-threatening.
“Donna told me that over the past two years she had an enlarging mass around the base of her right thumb, along the proximal phalanx,” says Dr. Jones. “In the clinical exam, it looked like it was a large mass 270 degrees around the bone. The MRI showed a mass ¾ of the way around the bone with an elevation of the blood vessels and nerves.”
The diversity of tissue substances in the hand such as fat, skin, tendons, and nerves allows many different kinds of hand tumors to develop in an array of ways including:
- A mole or wart
- In the soft tissues under the skin
- In the bone
Orthopaedic oncology is a subspecialty in orthopaedic medicine specializing in the diagnosis and treatment of various tumors (both benign and malignant) of bones, soft tissues, and musculoskeletal nerves.
What Are the Treatments for Hand Tumors?
There are two primary ways to treat tumors of the hand: observation or surgical intervention. Often, the most effective treatment is the removal of the tumor with surgery usually performed right in the doctor’s office. A pathologist will then be able to examine the tumor and establish its nature and type.
Other patients upon learning that a tumor is benign, may take a wait-and-see approach and live with the tumor as long as it doesn’t begin to interfere with their quality of life. Should the tumor change color over time, grow in size, and cause pain, a patient may have it re-examined by an orthopaedic oncologist to determine the best mode of treatment.
Due to the debilitating effects of the tumor in Donna’s hand, she and Dr. Jones elected to undergo surgery as soon as possible. “Dr. Christensen and I took her to the operating room about a month after I first saw her, and did a biopsy,” says Dr. Jones. “The biopsy during surgery revealed it to be a giant cell tumor of the tendon sheath which is a benign but locally aggressive tumor. In this case, it actually invaded the bone.”
“We took out all the soft-tissue components and then with a tiny curette reached in and took out the residual tumor inside the bone. We sewed Donna up and then had her go to occupational therapy.”
What Is the Recovery Like After Hand Surgery?

Donna Hands Post Hand Tumor Removal Surgery
The speed of recovery will vary for each patient depending on their medical and family history, and lifestyle. Having an experienced, skilled, and compassionate medical team in one’s corner is a key component on the road to full recovery. Most surgeons will stress to their patients that surgery represents just the first step to re-establishing full strength and functioning of the hand and following a qualified physical or occupational therapist is vital to complete the healing process.
“My physical therapy lasted about a month,” says Donna. “I did everything they told me to do; I did the exercises, and today I’m perfectly fine and back to normal. I don’t have any problems typing or writing, nobody sees a tumor anymore, and I’m very, very pleased.”
Dr. Jones was also happy to see Donna’s hand recover so well following surgery, particularly in the areas of feeling and blood flow. “Thankfully, at the last visit about a month after surgery, Donna had normal motion and full sensation and vascular supply to the thumb,” says Dr. Jones. “So she’s back to doing all the things she was able to do prior.”
After her successful hand tumor removal, Donna is grateful for all the work Dr. Jones and his staff put into her treatment and would wholeheartedly recommend him to anyone suffering from a similar condition.
“If I had been a little more proactive, it probably wouldn’t have been such an intense and long surgery,” she says. “I would say to anyone (needing help) to ask your physician to give you a referral for Dr. Jones and his team.”


